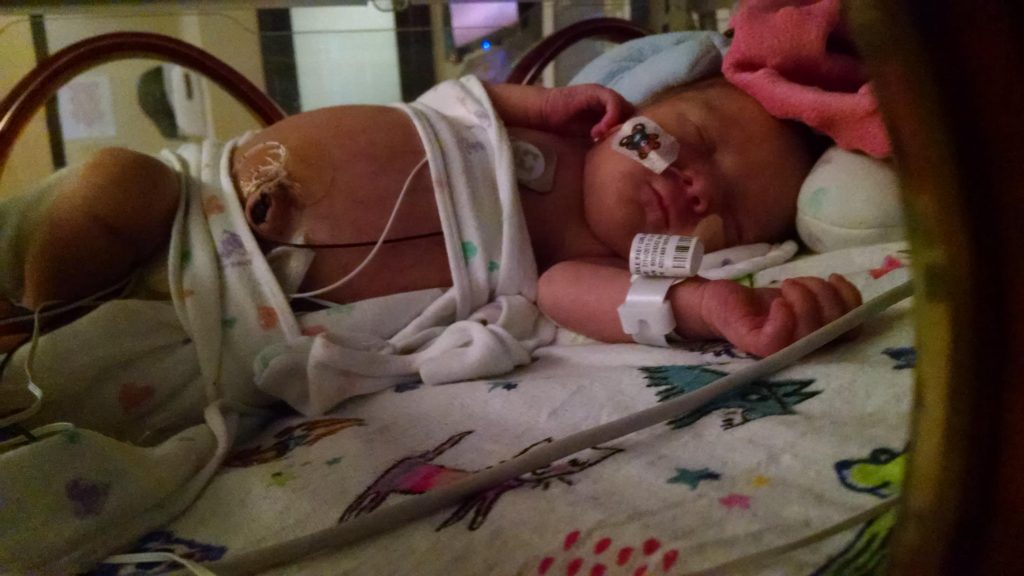
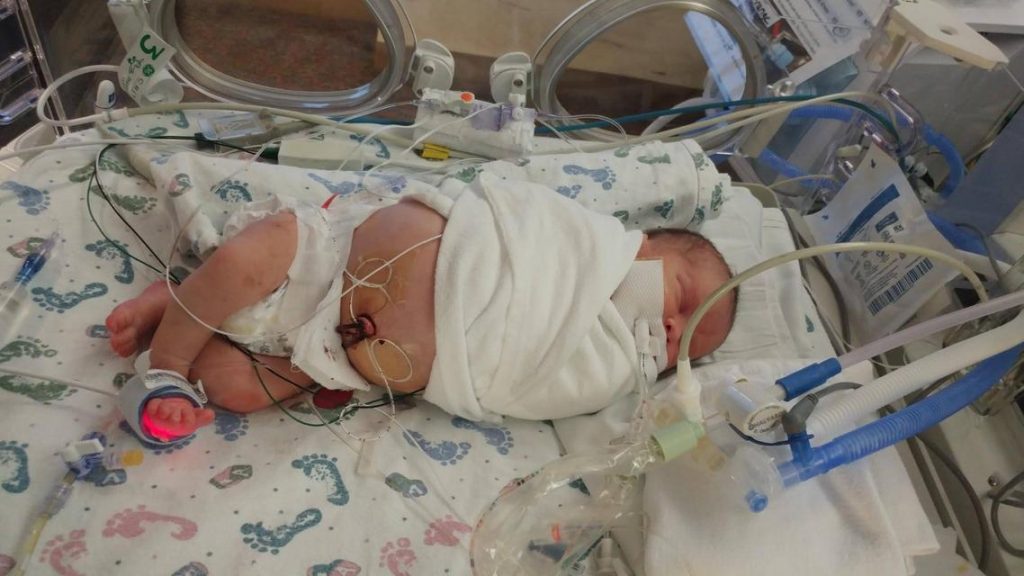
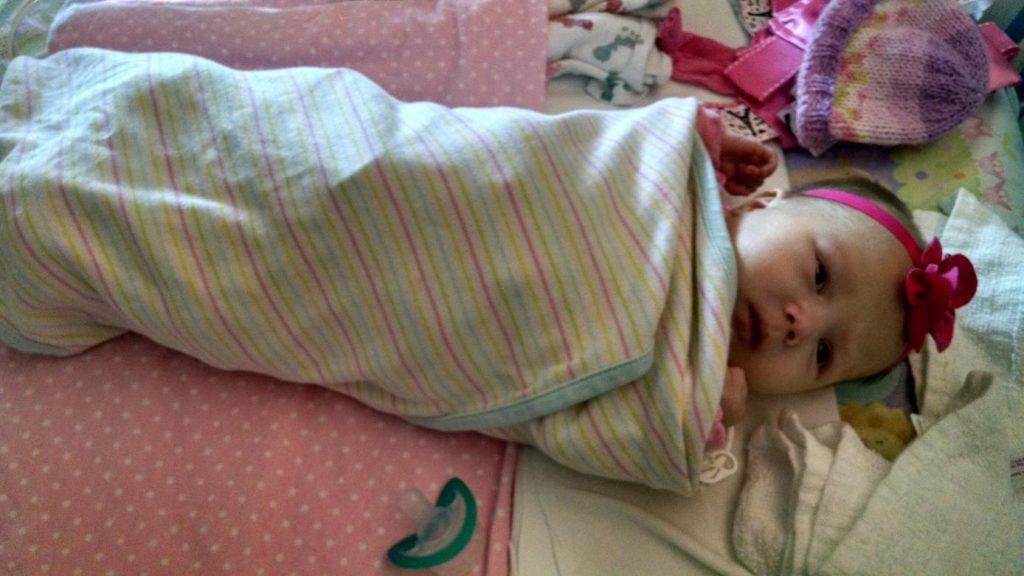
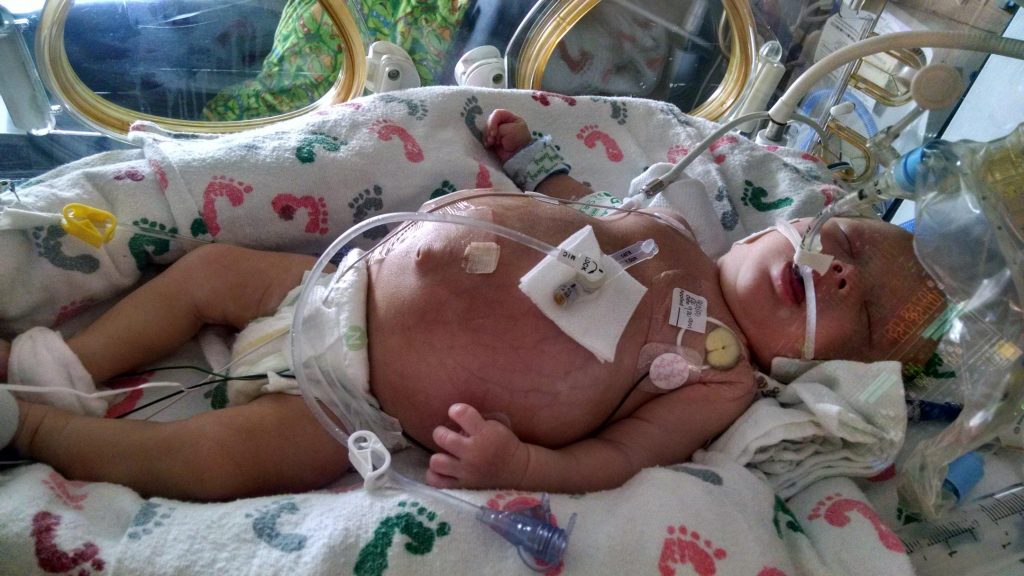
Before I became a transplant mom, I was a NICU mom, and as most of you know from talking to me personally or reading my posts here, I was a NICU mom three times over. There is no experience that changes you like having a child, but I think that having a NICU baby is an even more formative experience than regular parenting. I still get asked about my family’s time in the NICU reasonably often, so I thought I would write a little about it here.
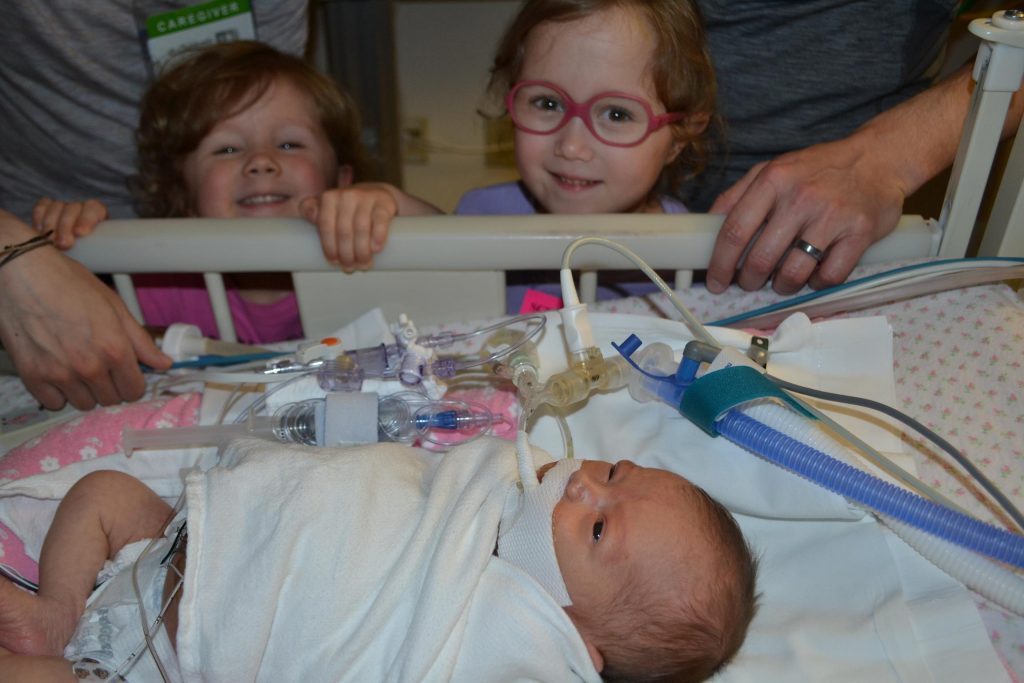
The first thing I will say is that having a NICU baby is overwhelming and scary, especially for the mother. As a mom, you do all the hard work of giving birth and at the end, you’re supposed to get the reward of holding and snuggling your baby. A NICU mom loses that reward when her baby is whisked away right after birth. The mom has to cope with all the physical changes her body is going through as she recovers from giving birth, plus the challenges of trying to get nursing/pumping established, plus going to the NICU from her hospital room. On top of the physical difficulties are the many emotions NICU moms experience. Your beautiful little baby was with you and a part of you just a short time ago and you were able to protect them and keep them safe. Now you can’t see them whenever you want and you must ask permission to hold them. You can’t protect them from pokes, hurts, and loud, scary noises. And you have to leave the hospital without them when you are discharged. I cried when I was discharged from the hospital and had to leave E in the NICU, and I distinctly remember walking around our apartment in a daze when my husband brought me home that evening. It felt so wrong to be somewhere without her. Likewise, it was so hard to see V transported from one NICU to another the day she was born and know that she wasn’t even in the same building I was. Even with M2, my third NICU baby, it was awful not holding him until almost 24 hours after he was born and then leaving him at the hospital when I was discharged. One of a mother’s base instincts is to protect her child, and that’s hard to do when your baby is in the NICU. As a mother, you feel scared, overwhelmed, and helpless. But these feelings aren’t just experienced by moms. Fathers feel them too. My husband did. He didn’t have the challenge of physically recovering from birth, but he did have the challenge of supporting me in my physical recoveries and supporting me through all the emotional and hormonal changes I went through. There are definite differences between the experiences of NICU moms and dads, but both parents go through a lot.
Now, some of the following advice and anecdotes may sound familiar, as some of these things I’ll write about as a NICU parent I’ve touched on before for transplant families. The reason I was able to write about them for transplant families was because our NICU experiences were so formative for us. Transplant was a different ball game than NICU life to be sure, but there were so many similarities that we took what we learned in the NICU and used it to our best advantage with transplant.
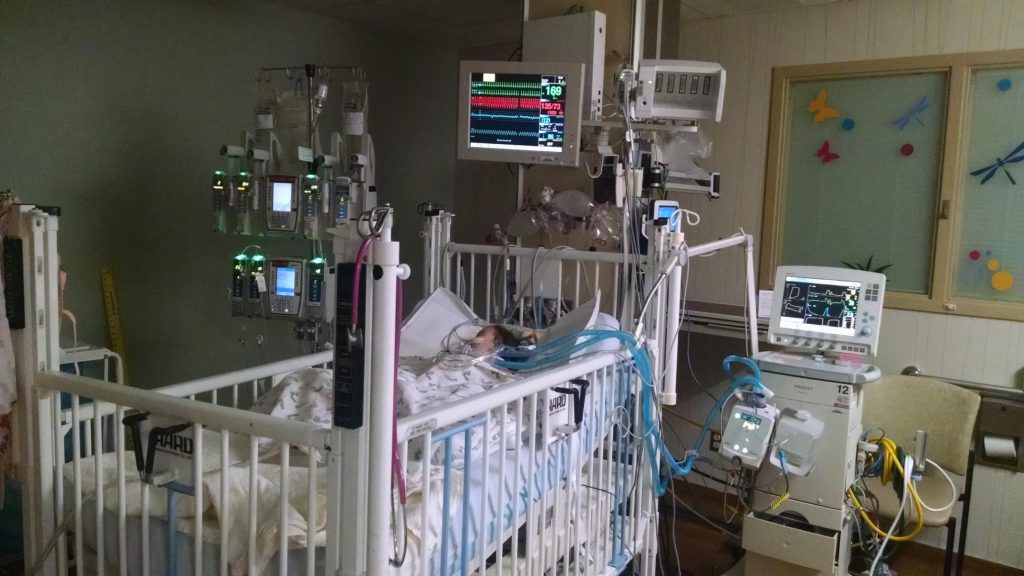
When you have a NICU baby, it’s overwhelming to be immediately immersed in a medical world with many new faces around you, alarms and monitors constantly sounding, and words spoken that might mean nothing to you. It is completely ok to feel this way. Most doctors and nurses know this and try to make it as easy as they can for parents. So what I will tell other new NICU parents is to take advantage of the white board in your baby’s room with all their daily vital information and the names of all the providers for that day. Ask your nurse any questions you have. If you aren’t getting the answers you need, keep asking your questions of multiple people until you do. Write things down in a notebook or on your phone to look up later, or to ask the doctor about when you see them. It is also perfectly acceptable to ask for options in care plans. You might not have all the answers or understand everything that’s going on, but you are still your baby’s parent and first advocate.
We were very blessed to have our babies in two outstanding NICUs with dedicated and amazing staffs. There are many nurses who became like family to us. We still think of them fondly and often, and we remain forever grateful to them for all they taught us about advocating for our kids. That being said, there might be times when you need to speak up about something to your nurse. Maybe that’s asking to turn down the volume on alarms or to take vitals at a different frequency, if possible. Maybe you’d like to do certain cares with your baby. Maybe you’d like the chance to speak with the doctor if you missed rounds. You’ll never know unless you ask. Most nurses are awesome – they are there to care for your baby but they are also there for you too. If you end up with a long NICU stay like we did (seven and a half months for E), then you will likely meet tons of wonderful nurses who will be friends in your corner. But there can be times when nurses and parents don’t get along the best, so if you as a parent run into this situation, know that you can ask to speak with the charge nurse about your child’s nurse too. You can ask for specific nurses who have given great care or ask to avoid nurses who might not be the best fit for your family. The charge nurse may not be able to honor your request, but you can at least ask. Hospital life is hard and nurses do their best to make it as easy as they can for families.
One of the things that helped us the most with E and M2 in the NICU was establishing routines for both home and hospital. We would set a time that we would like to be at the hospital (once I was discharged) and then would go at that time and be there until bedtime for each baby. Then we would come home, eat if we needed to, and do whatever quick chores needed to be done at home before going to bed. My husband was a huge help to me while I was pumping and nursing by keeping me fed and helping me wash my pumping supplies. We usually saved major household chores for the weekend before going to the hospital on those days. When we were at the hospital, we quickly got involved with cares. Doing this was a great way to connect with our babies, learn the hospital routine and terminology, and get to know our nurses.
Another thing to establish is a line of communication for family and friends. When your baby is in the NICU, your first thought is always for the baby and it can be exhausting to respond to multiple requests for updates from well-meaning family and friends. At first, my husband and I would both send text updates as we were able. When it became clear that E’s time in the NICU would be very long, one of us would send a group message to each of our families at the end of a very eventful day or after a surgery. When things weren’t serious, one of us would send a group message with updates every few days or every week. Some families post updates on social media or Caring Bridge sites that can be set up. Other parents designate one family point person they update and then that family member updates other family and friends. My best advice is to find a method that works for you and go with it. Don’t fret over responding to each text, voicemail, or message.
It can be very hard to ask for help when your child is in the hospital. I always felt that I didn’t want to be a burden to anyone. But it’s ok to ask for and receive help if you need it. NICUs have so many wonderful resources for parents – nurses, CNAs, therapists, social workers, even other previous NICU parents. Support is there when you need it. For example, NICUs have wonderful resources for nursing mothers. Social workers are absolutely wonderful at answering questions about insurance and programs for arranging care at home. Previous NICU parents often offer support groups. Therapists offer music therapy and techniques for helping bond with baby, along with helping baby meet physical, speech, and occupational milestones. We had family bring us meals and snacks we could take to the hospital, and my work colleagues arranged a weekly meal train for us while E was in the NICU. Still other friends offered to mow our lawn, run errands, get groceries, and clean for us. These offers of support were so helpful to us and enabled us to focus on our babies.
One of the things I heard often as a NICU parent was “remember to take time for yourself.” This advice is so hard to hear when you’re worried about your baby and want to spend as much time as you can with them. I found it extremely unhelpful, but I will recommend that you look after your health too. Try to get the rest you need when you’re at home. Getting run down and sick and having to miss time with your baby is no fun. It happened to me just once – I got a cold and needed to miss a day with E. Then I had to wear a mask for the rest of the week when I visited her. (Pre-pandemic, of course.) If you need an emotional pick-me-up, take friends up on an offer to get lunch – whether that’s at the hospital or at a restaurant close by. When E was first in the NICU, I often had friends and family who stopped by to visit us and then would take me to the cafeteria for a quick bite. It was just the right amount of support and respite that I needed.
Lastly, if you are a NICU parent now, know that it will take time to adjust to NICU life and time to adjust to home life once your baby is discharged. We had to get used to all kinds of equipment, monitors, IV and pump alarms, and dialysis machine sounds in the NICU. Then we heard phantom alarms at home for a long time after E didn’t need her various machines any more. Likewise, know that it will also take time to process all the thoughts and feelings you have. There is no way to fully prepare for a NICU stay, even when you know it’s coming. We thought we were prepared for both V’s and M2’s NICU stays since we were seasoned NICU veterans, but it was an adjustment for us with both of them just the same. There’s also no way to prepare for the crushing emotional blow of seeing your baby hooked up to machines, poked, prodded, and sometimes needing the use of a feeding tube or oxygen. Hang in there. Put one foot in front of the other and take it one day at at time. Celebrate the all the milestones. NICU life is a marathon, not a sprint. It’s very hard, but it teaches you how strong babies are and what a gift each day truly is. And over time, you will see that it makes you a stronger, more compassionate parent.