Recently, I was asked to be part of a support group for parents of kidney kiddos, so I’ve been reflecting a lot more on our family’s experiences – what we felt, what helped, what stressed us out, and what we wish could’ve gone a different way. Here is some advice I’d like to share with non-transplant families who might know a family about to go through the transplant process.
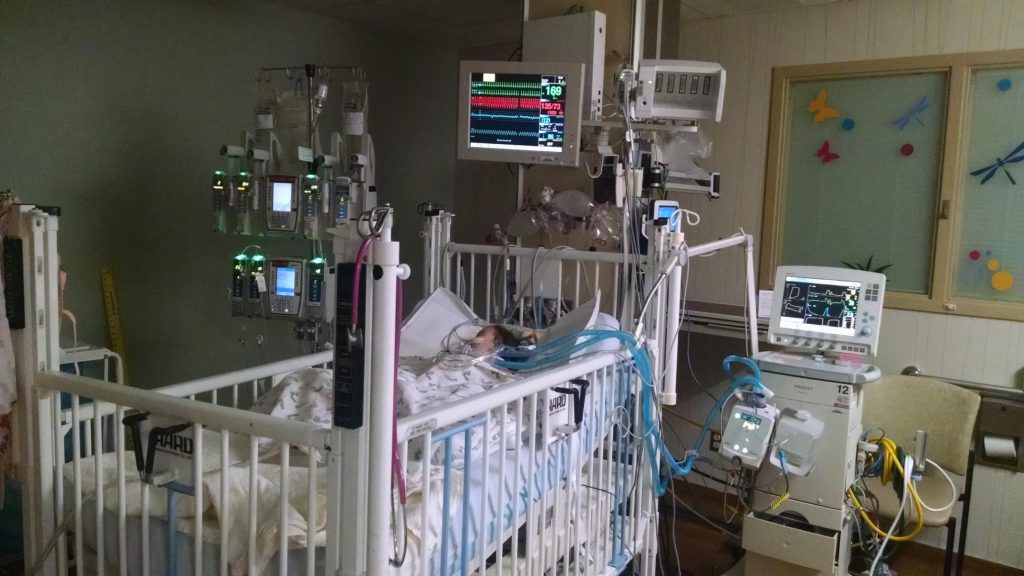
Don’t ask if the family is excited for transplant. That’s a weird and hard question to answer, and I would say it’s also an insensitive one to ask. I understand that you might be struggling to find something to say or that you might have completely good intentions, but just don’t ask this question. It’s not helpful in any way. Instead, ask the family (or future transplant kid) how they feel about transplant so they can say whatever they feel. When E’s transplant was imminent, my husband and I had quite a few well-meaning people ask us this question and we were always shocked by it. Yes, we were excited for the prospect at a more normal life a transplant would give E, but we knew the surgery is a complicated one that carries many risks for both the donor and recipient. In our case, we didn’t have just E to worry about – we worried about my husband’s sister too, who is E’s living donor. We also knew what other transplant families and medical professionals know but many outside the transplant community don’t – a transplant isn’t a cure for whatever disease or condition that caused the transplant to be necessary. A transplant is a treatment and carries its own side effects. Then there is the fear of making it successfully through the surgery only to have the patient’s body reject the transplanted organ in time. We transplant families live in fear of rejection, even if that fear is tucked away into a corner of our brains most of the time. So rather than being excited, our family felt a mixture of hope and fear leading up to transplant.
Another reason you shouldn’t ask a family if they are excited for a transplant to happen is that many patients don’t receive organs from a living donor. Many receive organs from a deceased donor. I can’t speak from personal experience on this front since E’s transplant came from her aunt, but we do have a dear friend who received two life-saving transplants from a deceased donor. He is so grateful for the second chance at life his transplants gave him, but he also had to work through grief for his donor, his donor’s family, and for the part of him that he lost. For the patients and families who receive transplants from deceased donors, I imagine it’s hard to be “excited” when they know how much another family hurts from losing a loved one.
Something else to avoid saying to a family soon to go through the transplant process is “I know how you feel” followed by whatever situation you’d lived through that you think must be comparable. Again, I’m sure you have good intentions and just wish to express your sympathy. BUT, unless your family has lived through the transplant process, you do not know what the transplant family is going through or how they feel. Even if you’ve lived through a serious medical condition, you can’t know what the transplant process is like unless you’ve lived it yourself. What I’ve found to be helpful is when someone has said a version of this to me: “I can’t imagine what you must be going through.” Honestly, sometimes that’s all that needs to be said.
You might wonder what you can do to help a family before, during, and after an organ transplant. That’s great! Please listen when I say the best way to offer help is NOT to ask the family, “How can I help you?” or “Can you tell me what you need?” A family going through transplant already has more than enough on their minds to worry about, and you asking them to identify specific needs so you can help them just amplifies the stress in most cases. And speaking from experience, sometimes a family doesn’t know what will help them the most until the transplant happens. The best advice I can give for anyone wanting to help a transplant family is this: offer them food or to run errands for them. Some of the most helpful support we got during E’s transplant was from friends and family who just made food and dropped it off at our house or who sent us gift cards to order carry out. Still others sent or dropped off snacks we could grab when we came home or throw in our bags when we went back to the hospital. During several of our family’s hospital stays, some of my very best friends have offered to go to the grocery store for us, do our laundry, or even mow our lawn. They wanted to do whatever tasks they could take on that would allow us to spend more time at the hospital.
If the COVID prevention measures ever go away, I would also recommend offering to visit a transplant family when they’re ready. I am in no way advocating for interruption of a patient’s or family’s recuperation time. Please be mindful that recuperation is stressful and scary and the infection risk is real. But sometimes the caregivers of a transplant recipient need a respite from the constant vigil kept at the patient’s bedside. During various hospital stays, I’ve had friends come to the hospital to take me to lunch for an hour while E’s nurse stayed with her. We had family members stay with E for a hour or so at a time during her transplant recovery so we could go home to shower, get something to eat, or take a nap. And lastly, we had friends and family just come keep us company for a little while to help us take our minds off our worry. But remember to ask before you plan to visit and don’t be offended if the answer you get is “I’m sorry, but this isn’t a good time.” The transplant family knows you want to support them, and there will be other times when you can see them that might be safer or less stressful for them.
Now some advice for interacting with a transplant family after the transplant. Remember that the transplant family is figuring out their new normal. A transplant recipient has a lot of medications to take, follow-up appointments to go to, labs that need to be taken, and potentially even therapy to get through. It may be a while before anyone in their family is comfortable receiving visitors at their home or up to going out. Be respectful of their time commitments and choices to stay home, as each healing process is different. Please also understand that their attitude toward sickness prevention will change, as they need to protect the patient’s transplant. Please don’t be upset if the transplant family doesn’t attend a celebration or social event you host. They might not feel comfortable attending a crowded event. Or please don’t be offended if there are new rules established for visiting their house. We regularly enforce the rule of not visiting our house during flu season if you don’t get a flu shot. We are also not shy about asking if friends and family have gotten their shots. And I would hope that by now, our family and friends know that many times we aren’t in attendance at events not because we don’t want to be there, but because we are looking out for E’s health by not exposing her to other people’s germs.
Lastly, give the transplant patient and family some time to process and work through the myriad thoughts and feelings they might have after the transplant. If they want to talk and vent, let them do it. But if they want to talk about something completely different to take their minds off the overwhelming thing they’ve just gone through, by all means, help them in whatever way you can. Maybe this is bringing up a silly book or joke you read, showing them a goofy viral video, or even just discussing their favorite sports team’s recent performance. I promise that if you are truly considerate and keep the transplant family’s needs ahead of your desire to help them, you will help them when all’s said and done.