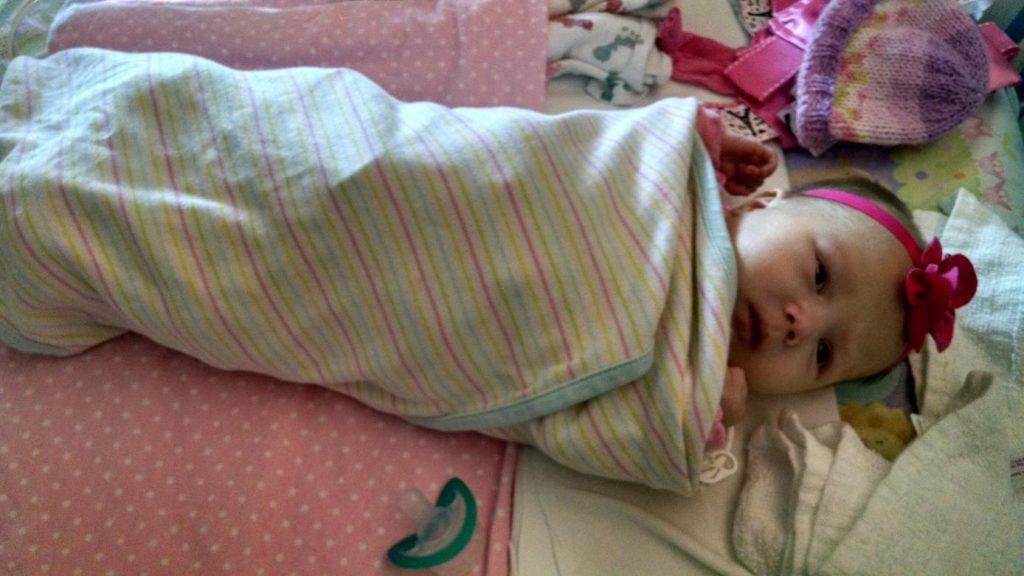
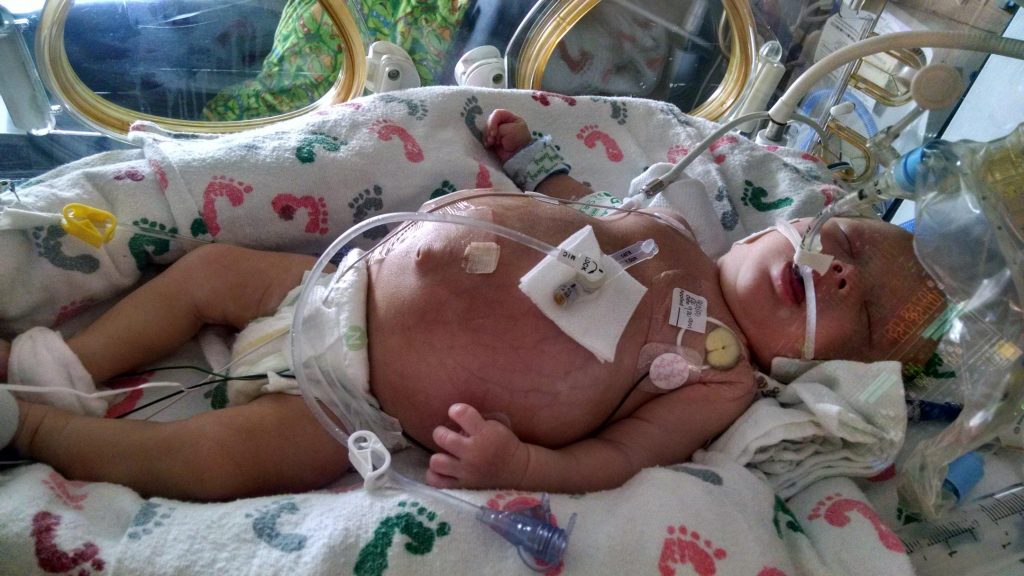
It’s been a busy month and a half at our house since my last post. Between summer get-togethers, the 4th of July, important family news, a week-long fishing trip for my husband, a major power outage, a birthday party, and then a pharmacy situation, it’s been a bit hectic. That doesn’t mean that I’ve been without food for thought for this blog though! So, let me talk about a couple of recent events in our family that illustrate my overall theme of advocating for your child.
One of my most recent posts discussed how COVID isn’t over for us just because the mask mandates are over. At the end of June, NPR published this story that emphasizes how much we should be protecting the immunosuppressed people in our society to help conquer COVID faster. Immunosuppressed people are less likely to develop an adequate immune response to the COVID vaccine due to the medications they’re on and so most likely need more than two doses to have some antibody protection from COVID. Research is also showing how immunosuppressed people can spread variants because it takes them so long to develop effective antibodies to the virus. So, the article argues that we should be doing everything we can to protect the immunosuppressed people around us. I shared this article on social media because I firmly believe that everyone should be getting the vaccine if they can. If one can’t get the vaccine for whatever reason, then that person should be doing everything they can to protect those around them by practicing social distancing and masking up. This is what I’ve been saying to those around me and this is what we’ve been doing for E. Yes, it stinks that E can’t go to the zoo, that she can’t go over to friends’ houses to play inside, that she can’t go to family parties if not everyone’s vaccinated. But my job as her parent is to protect her the best that I can, and sometimes, the best thing for me to do is to keep her home to keep her safe. Other times the best thing I can do for her is to speak up and educate those around me. How can I expect someone to respect my point-of-view if they don’t know my experience and they don’t know how their actions affect E?
When my husband was off on his fishing trip, I saw a friend post on social media about a medial ID bracelet she’d purchased for her daughter. She posted a picture of a pink and white silicone bracelet that looked like it would suit E very well. I’ve been wanting to get E a medical ID bracelet for over a year now. I felt that she’d be safer when we go out or if she’s not in our care if she had one. All the products I’d seen though were too bulky, too grown-up, too big, or too expensive, so we decided to wait a while to buy one, especially since we weren’t going out much thanks to the pandemic. When I saw my friend’s picture of her daughter’s bracelet, I knew I had to check out the Etsy shop she purchased it from. Turns out, I.C.O.E. Bracelets had just the type of bracelet we wanted and I ordered one for E. E had fun choosing the color she wanted and I was glad I got all the information I needed engraved on the bracelet. So now when E goes out, whether with us or anyone else, she’s going to wear the bracelet with this information on it:
Kidney Transplant
Anti Reject-Meds;
No NSAIDS
ICOE (in case of emergency):
[Mom’s phone number]
[Dad’s phone number]

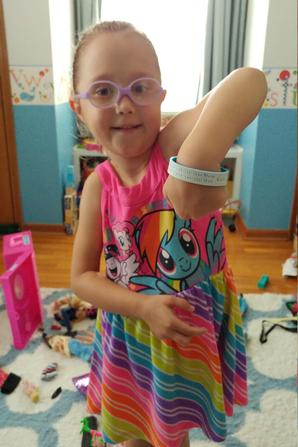
You’re probably wondering what a medical ID bracelet has to do with advocating for your child. Well, think of it this way: it’s a way for me to communicate to other adults enough about E to ensure she’s well taken care of in case she’s ever in an emergency situation and I’m not there. It’s a way for her to tell other people about herself too – whether she’s educating an adult in an emergency situation or exposing a peer to transplant kiddos for the first time. It can be both a life line and a conversation starter for her when she’s out and about. And the older she gets, the more she’ll be away from me, so it’s peace of mind for me that I’m giving her information she needs no matter where she goes.
The biggest, most stressful situation that happened lately that reflects my theme of advocating for your child came about thanks to CVS Specialty Pharmacy. On July 14th, I reordered one of E’s twice-daily anti-rejection medications. I specified delivery for Friday, July 16th and didn’t think twice about it…until the afternoon of July 16th arrived and I hadn’t gotten any shipping confirmation emails about E’s prescription. So I contacted CVS Specialty and asked for an update. The answer I got was that the med would be delayed indefinitely because a prior authorization was needed by our primary health insurance company. Until that prior auth was signed by E’s doctor and received by the insurance company, CVS Specialty would not fill E’s order. Then the message said that the prior authorization request had been sent to E’s doctor and that CVS couldn’t tell me how long the process would take. Our regular transplant nurse coordinator was out of the office that week, so I immediately fired an email away to one of the other nurse coordinators explaining the situation and asking her to please follow up on the prior auth right away. Then I calculated how many doses I had left of the anti-rejection med in question and called our transplant office in case the nurse coordinator I emailed was out of the office too. The nurse coordinator who called me back right away assured me that she would work on the prior auth with the doctor right away and that she would get everything lined up at the hospital pharmacy in case we needed emergency doses of the anti-rejection med. I then sent a firmly worded message back to CVS Specialty demanding to know why a prior authorization was needed since E’s prescription didn’t expire until January 2022 and we’d just had one sent in January 2021. I also demanded to know why I wasn’t notified that E’s prescription would be delayed, (especially when I have to specify how many doses of a med we have left when we place a refill order). The message I got back stated that our insurance company rejected the anti-rejection med because they determined it was “not medically necessary.” CVS could not tell me how long the process would take to resolve and they apologized for any “inconveniences” the delay caused me. I was incensed. E had enough doses of the med to get her through the morning of July 19th (a Monday), after which we’d be completely out. Thank goodness I’d spoken to the nurse coordinator right away and arranged for possible rescue doses. How could all the people at CVS Specialty who worked on E’s refill not realize that by not communicating to me about the delay they ensured we would run out of doses for her and that missing a dose means risk of rejection for her?!
I was so upset by this turn of events that I decided to call CVS Specialty on Saturday morning to follow up on the prior authorization request, as I knew from earlier this year that they worked on Saturday mornings. Well, turns out, CVS has recently changed its Specialty business hours, so only emergencies are handled on Saturdays now. Ironically, the first gal I spoke with to explain my emergency – that my daughter would run out of anti-rejection meds by Monday – told me that my emergency WASN’T an emergency. According to her, an emergency would be if E was already out of doses. Not a good omen to start another day. I demanded to talk to the on-call pharmacist. When I finally talked to the on-call pharmacist and explained the situation, she agreed that we had an emergency and put me through to the escalation team so that E could get meds right away and not miss a dose. The gal I then spoke to on the escalation team apologized and said CVS would “definitely” get the anti-rejection med to us by 9 p.m. CST on Monday, July 19th to ensure E wouldn’t miss a dose. She canceled an order set to arrive on the 20th, verified that there was no copay associated with the order, and informed me that a claim associated with the prior auth had been satisfied. She then told me that someone with CVS would call me either later Saturday or Monday morning to verify the shipment. After speaking to both the pharmacist and the escalation team member, I felt a little better – which was good considering that July 18th was E’s sixth birthday party and July 19th was her actual sixth birthday. I didn’t want to spend both days worrying about procuring meds for her.
We had a nice time at the party the next day on the 18th and it was a great day for E. For her birthday on the 19th, I told her she could decide all our meals and we would play whatever she wanted to play that day until her dad got home and she opened the rest of her presents. But by 9:30 a.m., that plan sort of went down the drain. That’s when CVS Specialty called to talk to me about getting E’s med to us “as soon as possible.” The gal I spoke with said she’d work on it and get back to me with an estimated time of delivery. I was annoyed after the call since I was expecting this call to just confirm delivery, as per my conversation with the escalation team member on Saturday. At 1:45 p.m., the same gal I’d spoken to at 9:30 – a member of the resolution team – called me back to tell me that the earliest she could get E’s med to us would be 1:15 a.m. Tuesday(!). When I told the gal that this “resolution” was unacceptable because it meant that E would miss a dose and that I would have to go to our hospital to procure rescue doses, the gal said she was “sorry for the inconvenience” it caused us. I then asked why there was a discrepancy between what the gal on the escalation team promised me for delivery by 9 p.m. Monday and the actual arrival time of 1:15 a.m. Tuesday, and the gal told me that she didn’t know what the escalation team member had promised me since they were on different teams and she could only offer what she could offer. I then asked to speak to her supervisor. She told me there was no one else I could speak to because she was a member of the resolution team. So then I asked if she could tell me why no one from CVS had contacted me to inform me of the prior auth request the previous week. She told me that they don’t normally do that because they communicate with the doctor’s office and it’s the doctor’s responsibility to turn in the information for the prior auth to insurance as soon as possible. Then she told me there was nothing I could’ve done to speed the process along if they would’ve contacted with me. I told her I begged to differ with her – if I would’ve known about the prior auth request I could’ve worked with my transplant coordinators to alert the doctors to the prior auth request sooner and could have potentially avoided running out of meds. The gal also told me that she started working on the request as soon as she got in to work. I find this hard to believe considering that CVS Specialty is based out of Pennsylvania and therefore on Eastern time, while I am in Central time, and based on the time I got the call, it was already 10:30 a.m. in Pennsylvania. If my emergency request with the escalation team from Saturday had been taken seriously on Monday, then the gal with the resolution team should’ve only had to arrange shipment right away when business hours started on Monday. So where was the breakdown between teams here? What good is an escalation team if they don’t actually speed things along? What good is a resolution team if the resolutions they devise don’t actually provide resolution to the problem? What good is a national patient portal if teams from different departments don’t communicate with each other and work together? I informed the gal that CVS Specialty is the worst specialty pharmacy out of the three I have worked with and I was extremely dissatisfied with the way our current situation was handled. The gal then asked if I needed to speak with a pharmacist. When I answered no, she told me that she would send me the tracking information for E’s shipment.
So rather than playing with E and making her favorite supper for her birthday, I made two different phone calls to the outpatient pharmacy at our transplant hospital after the second phone call with CVS and arranged to pick up emergency doses later in the day. When my husband got home, the prep work for supper was done and I informed him he’d have to throw everything together, and we had E open the rest of her birthday presents before I had to leave for the hospital. When I got to the hospital pharmacy, I had to wait just five minutes before picking up E’s rescue doses, which one of the pharmacists apologized(!) for not having ready sooner and which was not billed to insurance at all. The hospital pharmacy even gave me more than we needed – just in case. Yes, our hospital has a vested interest in making sure E gets the meds she needs since she is their patient, but what a difference in customer service between our hospital pharmacy and CVS Specialty! We were treated like people with an emergency situation at our hospital, whereas CVS Specialty treated us like we were random numbers. As I made my 15 minute drive home from the hospital, I wondered what we would’ve done if we lived in a rural area and were hours instead of minutes away from our hospital pharmacy. What would we do without our amazing nurse coordinator who ensured the rescue doses would be waiting for me?
After supper we played outside with the girls and enjoyed home made ice cream on the deck before bed time. Wouldn’t you know that the tracking number the resolution team member gave me for E’s shipment didn’t work? To prevent the doorbell from waking everyone up that night, I decided to sleep on the couch until the courier arrived with E’s med. Good thing I made that decision because the courier didn’t arrive until 2:45 a.m. and I didn’t get to bed until after 3. Naturally, I was tired the next morning and wasn’t at all up for any more nonsense. A representative from CVS called me a little after 8 to make sure the courier had delivered E’s med with no problems. When I shortly replied yes and told her at what time the med arrived, she asked if there was anything more she could do for me. I ended up having a half-hour long conversation with her about everything that had happened and I asked her what the procedure was at CVS that E’s med could have been delayed from one department to another. I also asked how a prior authorization could have been required for an existing med that had a current prescription. The representative was very apologetic, listened to my version of the story, and took notes to call the supervisors of the previous representatives with whom I’d spoken. She looked into E’s online patient portal while I was on the phone with her and saw that the med had been billed incorrectly – so no prior authorization had actually been needed! What happened was that the person/people who tried to bill the med to insurance didn’t do the billing in the specific way needed for this particular med and when they encountered a problem, they didn’t ask for help. You can imagine what I felt when I heard this. The representative repeatedly told me that I didn’t deserve to be treated the way I had been and that meds should not be this hard to order. She promised to find me a dedicated person to place orders with in the future who would know how to handle E’s anti-rejection meds and she promised to follow up with me the next day to update me on the progress she’d made to guarantee a medication delay never happens for us again. Well, that representative who actually demonstrated kindness to me for the first time ever from CVS Specialty ended up never calling back. Perhaps she wasn’t as genuine as I thought she was. Or perhaps her supervisor prevented her from doing more to help me. I don’t know. That doesn’t mean my fight is over though. As per the advice I received at the beginning of the year from another transplant mom, I’m going to file a formal complaint with our insurance company against CVS Specialty. Our insurance company needs to know that we weren’t well-served by CVS Specialty and because of CVS, E could’ve gone through a much more serious situation – one that could have forced our insurance company to pay hospital bills instead of covering a preventative/maintenance medication. I am also doing more research to see if there are other ways for us to get around using CVS Specialty as our pharmacy.
Besides raising my blood pressure, this latest episode with CVS Specialty demonstrates how important it is to be your child’s first and best advocate. Being an advocate is the biggest lesson I’ve learned since the day E was born. I can’t count the times I’ve spoken up for E and I can’t imagine what would’ve happened to her had I not done that. For example, we surely would’ve run out of meds due to pharmacy problems many times if I hadn’t been on top of the issues and asked to speak to supervisors, done my own research, and worked with E’s doctors and nurses. I have spoken up about delays in E’s transplant team communicating with us. My husband once called out a prescription error on a doctor’s part that could have been fatal for E if he hadn’t been paying close attention to her medications. We fought for specific goals and treatments for E when she was just a baby in the NICU. I just can’t emphasize enough how important it is to advocate for your child’s health.
Loving your child comes naturally, but speaking out for them doesn’t happen automatically for every parent. If speaking up doesn’t come naturally to you, remember that no one knows your child like you do and your gut instinct is usually right when it comes to your kid. This advice applies to parents of healthy kids and medically fragile ones. If you aren’t getting the answers you need from your child’s doctor, seek a second opinion. Ask questions until you receive the answers you need. If a treatment option isn’t right for your kid, say so and don’t rest until you find something that works. If you feel your kid needs speech/physical/occupational/emotional therapy but your school district or insurance won’t help, ask your doctor for help, reach out to other parents to see what avenues they know of, or ask to be pointed to a social worker. Don’t take no for an answer when it comes to your child’s health!
Know that your child sees what you do for them. By advocating for your child, you show your child they are worth fighting for. You show your child what it looks like to stand up for someone or something they believe in. You show your child how to advocate for their own health someday. Keep in mind that there are ways to be firm and advocate for your child without being rude. Also remember that sometimes the best thing you can do is admit you need help from someone else to get the answers you need. Your child sees these things too. There are times when a child has to learn that not everything can go their own way. But when it comes to health issues, no child should have to go it alone or without, and they should know it’s ok to ask for help. So be your child’s tireless, unwavering, strong advocate and teach them to stand up for themselves in the process.
So, you can see that I practice what I preach. In all these scenarios I’ve laid out, I advocate for E one way or another. I work to educate and inform others about ways they can help keep people like E healthy and safe. I take measures to provide for E even when I’m not with her. Lastly, I work to take care of E and empower her by always standing up for her health. Hopefully my actions and example will encourage other parents to do the same for their kids.