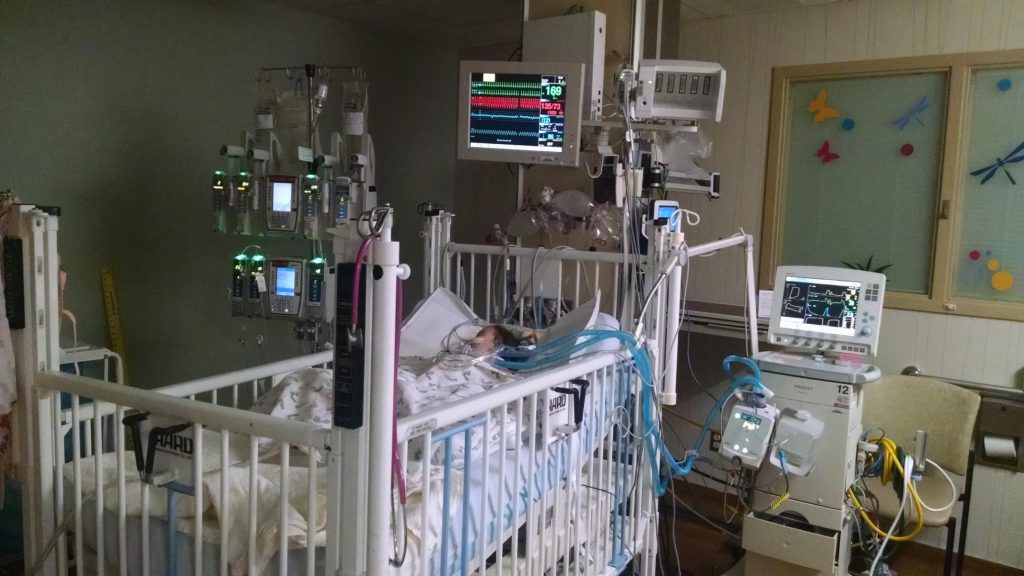
Now that we’ve gone over how non-transplant families can interact with a family going through the transplant process, I’d like to share some advice for families about to go through transplant. Our official transplant education at our daughter’s transplant center was top-notch, but it still didn’t cover everything. So here’s what I want prospective transplant families to know.
Before transplant:
Get your ducks in a row. Even if you’re waiting for the call that an organ is ready and you don’t know when surgery will be, get as much in order ahead of time as possible and rest when you can. You’re going to be incredibly busy and you probably know hospitals are not good places to get rest. Arrange childcare for other children, plan how you’ll let your boss know you’ll be off work, and do any FMLA/PTO paperwork in advance. Make a few meals you can throw in the freezer. You might even work out which family members or neighbors can check on your pets. Once you get the green light that transplant is a go, things will move fast. You’ll be so glad you’re prepared.
Don’t be shy about telling people they can’t come over (this goes for after surgery too). Let people visit who are truly helpful and supportive – those in your most trusted inner circle. You don’t need the stress of visitors who aren’t considerate of what your family is going through. Some of the best advice my husband and I got when we went to our birth education classes when we were expecting E was about visitors and it absolutely applies to this situation as well. Our instructor told the fathers to be the gatekeepers for visitors: if a visitor would stress a mom out after delivery, it is the partner’s job to protect the mom’s health and sanity by putting that visitor off until a later time. So, protect your family’s health and sanity by knowing your limits with visitors. All you need to say to someone is, “Now’s not a good time.” If the prospective visitor truly loves your family, they won’t be offended.
Have a designated channel of communication for updates about your kid. All of your family and friends are going to want to know how things are going. But one of the last things you need is your phone blowing up with hundreds of texts, missed calls, and voicemails that you feel you need to address. Decide ahead of time how you’ll communicate updates. Maybe one parent will send texts to another family member and that family member will get the word out via social media. Or establish group text threads for each parent’s respective extended families. Some hospitals allow parents to set up Caring Bridge websites and the like for families to post updates. If that’s something you want to do, decide which parent will write posts. Lastly, if you’re uncomfortable with family and friends sharing news about your kiddo’s progress in any fashion, say so. You have the right to control what information about your kid is shared and with whom that information is shared.

During transplant:
Don’t be afraid to ask questions and speak up for your kid. You are the expert on your child, even if you’re not an expert about transplant. If something doesn’t feel right, say so. If you have questions, ask them until you get answers you understand. If you don’t agree with a treatment plan, ask for alternative options. If a nurse, CNA, or therapist doesn’t have a bedside manner that you feel works for your child, ask to speak with the charge nurse. Be honest about your concerns and ask them for a different nurse or CNA the next day. Likewise, if you have a really great nurse, ask for that nurse to continue your care. My husband loves to joke about how my most protective Mama Bear instincts were brought out during E’s transplant by one Child Life Specialist. E was 16-months-old when she had her transplant and she wasn’t verbal at all. On top of this, we didn’t want her playing with a lot of communal hospital toys due to potential germ exposure, even if those toys are routinely and carefully cleaned. But we had one persistent Child Life Specialist who just wouldn’t leave us alone and wouldn’t take no for an answer when I firmly told her we didn’t need or want toys for E. We had everything we needed. Finally, I told our nurse we absolutely did not want any Child Life Specialists in E’s room bothering us. We also only allowed the minimum physical therapy for E since she wasn’t walking yet and felt the physical therapist didn’t understand where E was in her development. I do not feel one bit bad about speaking up for E in these situations. That’s what she needed from me. (And by the way, contrary to what my husband says, I don’t hate all Child Life Specialists. We actually know and like two really great ones at E’s Infusion Center.)
Be prepared for unforeseen complications. Complications could occur both before you leave the hospital and once you get home. No one knows exactly how a patient’s body will react to a transplant. In our case, E’s surgery went swimmingly, but her surgeon told us beforehand to prepare for the possibility that she wouldn’t be able to close E all the way. Thankfully, E’s new kidney worked right away, the surgeon was able to close E, and E’s incision remained infection-free. But once E was stable enough to move from the PICU to the general pediatric floor, we had trouble restarting her feeds and she vomited uncontrollably. It took several days to find the right balance of fluid and calories before the vomiting stopped, and E’s doctors told us the only reason they were keeping her in the hospital was to make sure she was getting the fluid and nutrition she needed. Once E was finally discharged after transplant, she ended up back in the hospital for an overnight stay two weeks later thanks to a concerning lab result. Thankfully again, the concerning result turned out to be lab error, but it was still an unforeseen complication.
Never stop praying. My husband and I have active faith lives and believe you are never truly alone if you pray. But sometimes it is hard to keep going in trying times, so let other people pray for and with you. Our parish priest came to the hospital to pray with us while E and her aunt were in surgery. That was such a comforting thing for us. We also found strength and support from lay ministers at the hospital. One man came to visit us who had also had a daughter in the PICU as a toddler and another lady happened to be a member of our parish community. You never know where support may show itself. If you’re not religious, that’s ok. It might still help you to talk to a hospital chaplain though. We’ve met quite a few hospital chaplains of various faiths and have found them all to be down-to-earth and wonderful listeners. They are often also trained counselors. So even if you’re not religious, a chaplain may offer you a sympathetic and supportive ear.
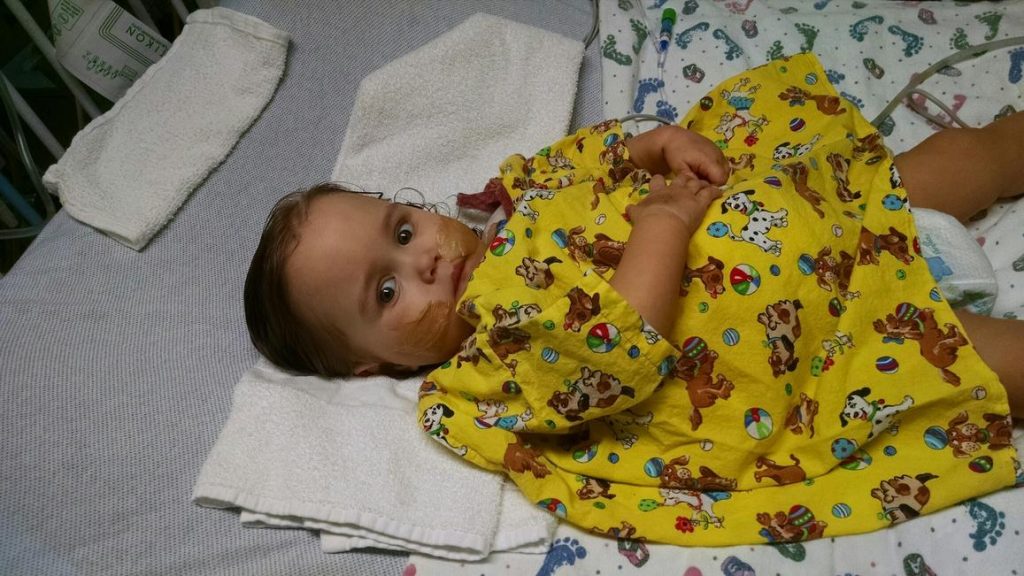
After transplant:
Post-transplant IS very different from the pre-transplant world. Many people will offer you advice on how to manage all the different appointments, medications, labs, and the like after transplant. But do what makes the most sense for your family. If you already have a system for appointments in place, awesome. Go with it. If you need ideas for new ways to manage meds, try one suggestion and if it doesn’t work, modify it to fit your kiddo and family. We have a nurse friend who gave us ideas on how to manage E’s transplant meds based on her experience with her husband’s transplant meds. We ended up modifying her advice to fit our family. For example, we separated medicines into different plastic snack bags and labeled them with the time they were to be given each day. Our friend’s husband separated his medicines by using colored snack bags. Still other people use pill boxes. Find what works best for your family and be open to changing your routine to fit your family’s needs over time. Meds, labs, and appointments will consume much of your lives for the first several months or so after your child’s transplant. After that, everything will taper down to much more manageable amounts – e.g., twice daily meds, labs once a month, appointments once a month, etc.
Divvy up responsibilities between parents. Both should know how to do everything, but neither should be responsible for doing everything. For example, when E came home from the hospital, my husband would make all her meds and formula, and I would give all the meds and deal with her feeding pump (filling bags, changing them out, and setting her pump). I interacted with E’s home health nurse during visits and took E to all her appointments, but my husband and I both gave baths and monitored E’s incision. My husband pays all E’s hospital and insurance bills, while I order meds from the pharmacy, make all calls to insurance, and interact with our social worker. Now that E’s older and she’s off her feeding pump, I make and give meds most of the time. One of the best things we did after E came home from the NICU was to write out her detailed daily schedule with doses and times for each med. We then made a list of the names and contact information for all E’s doctors, nurse coordinator, pharmacies, therapists, and social workers with our emergency contact information. We keep two copies of these documents in our home at all times – one copy of each document hangs in our kitchen and one copy of each is kept in a binder we send with E whenever she spends the weekend with her grandparents. Keeping multiple copies of these documents ensures that my husband and I have easy references to information in case we forget something or in case one parent needs to cover for the other. It also gives us peace of mind in case something happens to us and someone needs to step in and care for our girls. I’m sure detailed documents like these would also be super helpful for transplant kiddos who go to school or daycare.
If you’re a single parent, ask your social worker what programs your family might qualify for that could provide you with some in-home help, even if that’s temporary help. For instance, maybe your family qualifies for home health and a home health aide. Maybe your family qualifies for rides to appointments. Maybe your family qualifies for respite services. You won’t know what resources are out there until you ask.
NEVER be afraid to ask for help from your social workers or transplant office when it comes to pharmacy and insurance bills! Or when you need help navigating the complicated world of Medicare if you have a kidney kiddo like we do. That’s what these people are there for and they are life savers.
Lastly, never be afraid to call your transplant nurse coordinator, your transplant office, or pediatrician’s office if your child exhibits symptoms that concern you. You’ll be given lists of signs and symptoms to watch for, but if you’re not sure, go ahead and call. You’d rather be safe than sorry, and I’m sure your transplant coordinator or pediatrician is used to getting calls like yours. Everyone wants your kiddo’s transplant to be successful. Any time I had a concern about E during the two years or so after transplant, I always called her nurse coordinator first to let her transplant team know what was going on and ask how I should proceed. Now I am confident enough recognizing certain symptoms in E that I know who to contact first when we have concerns about her.
In the end, know that transplant is hard – but you will get through it. You and your kiddo have already made it this far and that’s half the battle. You can do this.